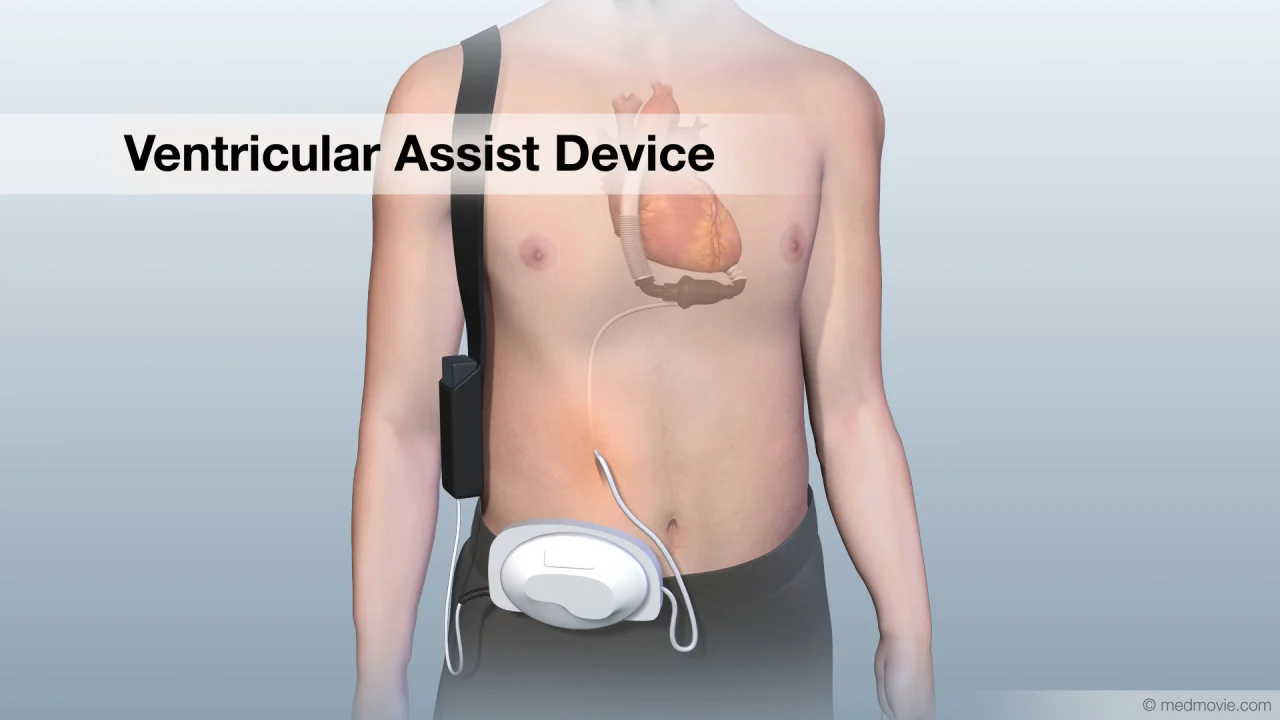
Ventricular Assist Devices (VADs): Advanced Mechanical Support for Heart Failure
A Ventricular Assist Device (VAD) is a mechanical pump that helps a weakened heart circulate blood throughout the body. It is used in patients with severe heart failure when the heart is unable to pump effectively on its own.
Why is a VAD Needed?
A VAD is recommended for patients with:
- Advanced or end-stage heart failure
- Weak heart pumping function (low ejection fraction)
- Patients awaiting a heart transplant
- Patients not eligible for transplant (long-term support)
- Severe symptoms despite medications
Types of Ventricular Assist Devices
- LVAD (Left Ventricular Assist Device)
Supports the left ventricle (main pumping chamber)
Most commonly used type - RVAD (Right Ventricular Assist Device)
Supports the right ventricle - BiVAD (Biventricular Assist Device)
Supports both ventricles
How Does a VAD Work?
- A pump is surgically implanted inside the chest
- It draws blood from the ventricle and pumps it into the aorta
- A controller and power source (battery) are connected outside the body
- The device continuously assists blood circulation
When is a VAD Used?
VADs are used in different scenarios:
- Bridge to Transplant – Temporary support until a heart transplant
- Destination Therapy – Long-term treatment for patients not eligible for transplant
- Bridge to Recovery – Short-term support until heart function improves
Benefits of VAD Therapy
- Improves blood circulation
- Reduces symptoms like fatigue and breathlessness
- Enhances quality of life
- Increases survival in advanced heart failure
- Allows patients to perform daily activities
Who is the Ideal Candidate?
VAD therapy is suitable for:
- Patients with severe heart failure not responding to treatment
- Individuals awaiting heart transplant
- Patients with poor heart function but stable overall health
A detailed evaluation is required before implantation.
Risks of Ventricular Assist Devices
As a complex therapy, risks may include:
- Bleeding
- Infection
- Blood clots or stroke
- Device malfunction
- Need for long-term anticoagulation
With proper care, these risks can be managed effectively.
Life with a VAD
Patients living with a VAD need to:
- Carry the external controller and batteries
- Follow strict hygiene to prevent infection
- Take medications (including blood thinners)
- Attend regular follow-ups
- Avoid water exposure to device components
Recovery After VAD Implantation
- Hospital Stay: Typically 2–3 weeks
- Full Recovery Time: Around 6–12 weeks
Recovery Tips
- Follow all medical instructions
- Learn device management and care
- Maintain a heart-healthy lifestyle
- Participate in rehabilitation programs
VAD vs Heart Transplant
| Feature | VAD | Heart Transplant |
|---|---|---|
| Availability | Readily available | Limited donor availability |
| Longevity | Long-term support | Permanent solution |
| Surgery | Complex | Highly complex |
| Medication | Lifelong anticoagulation | Immunosuppressants |
